Newest Treatment for COPD: Inhalers, Surgery, and More
Chronic Obstructive Pulmonary Disease (COPD) affects more than 16 million adults in the United States. That number is growing, which means our efforts to treat patients with the disease are also growing.
While there is no cure for COPD, there are continued advancements in treatment that allow patients to manage symptoms and prolong life expectancy in some cases.
Some use the term “emphysema” interchangeably with COPD, but that is simply one of the conditions that may be present with the disease (chronic bronchitis is another). We will take a closer look at the disease and its conditions and symptoms, its causes, and treatment and outlook for patients below.

WHAT IS COPD?
COPD describes a disease where airflow to the lungs is obstructed, with the obstruction caused primarily by inflammation. “Chronic” in the name implies that it is a long-term disease without a cure.
A COPD diagnosis can be overwhelming for many individuals, knowing they will suffer from the disease’s symptoms on a daily basis. However, there are also some treatments available to ease symptoms, and we will review those in more detail below.
The main cause of COPD is smoking, although it is possible to develop COPD from exposure to other irritants. The two main conditions indicative of the disease are emphysema and chronic bronchitis.
Emphysema
Emphysema occurs when cigarette smoke or other irritants destroy alveoli, a critical component of our lung function. Alveoli are where the lungs and the blood exchange oxygen; once oxygen passes through them, it travels to the rest of the body via the bloodstream. As you might imagine, when damaged or destroyed alveoli obstruct this process, the rest of the body suffers.
Chronic Bronchitis
Inflammation of bronchial tubes can lead to chronic bronchitis. This differs from acute (temporary) cases of bronchitis that may be associated with a cold or the flu.
Chronic bronchitis sufferers cough daily and deal with the unpleasant effects of mucus production.
When patients are diagnosed with COPD, they need to monitor their health closely for other possible complications. For example, the common winter cold or flu can be much more difficult to manage with COPD. Also, those with COPD are at a greater risk for lung cancer, heart disease, and other serious health issues.
COMMON COPD SYMPTOMS
When it comes to symptoms, COPD has a great deal of overlap with many other respiratory conditions. For example, wheezing, which can be present with COPD, may be caused by asthma.
Typically, COPD patients will experience many of the symptoms listed below, which should always be discussed with a doctor:
- Shortness of breath, while exercising or just going about daily activities
- A persistent cough
- Fatigue
- Increased mucus production
- Wheezing
- Frequent respiratory infections
- Bluish tint to lips or fingernail beds
HOW IS COPD DIAGNOSED?
The most effective tool physicians have in diagnosing COPD is a spirometer.
Spirometry, which is non-invasive, allows a patient to blow through a mouthpiece into a machine that measures both the amount of air blown out in the first second and how much a patient can blow out altogether.
These measurements, the forced expiratory volume and forced vital capacity, tell a physician just how severely your airflow may be obstructed.
Your physician may also order a chest CT or x-ray to determine if another condition may be causing your shortness of breath, such as pneumonia, a nodule on your lungs, or even a blood clot. These tests may reveal damaged lung tissue or other sources of airway inflammation.
One of the greatest challenges with COPD is that, in some cases, adults are initially diagnosed with asthma. Because both COPD and asthma have shortness of breath and wheezing as common symptoms of pulmonary disease, they can be confused, even by trained physicians.
They do share some overlapping treatments (such as the use of inhalers), but a proper diagnosis is crucial for the specific treatment each condition requires.
TREATING COPD
After a COPD diagnosis, your healthcare provider will work with you to determine the best treatment plan for your case. This will vary from patient to patient, taking into account the severity of the airway obstructions and other health complications, such as the presence of heart disease.
COPD will never go away; however, this does not mean a patient cannot continue to live an active life and find ways to treat symptoms effectively. The first and most important step is to quit smoking, which can slow COPD progression, help a patient respond better to treatments, and improve the patient’s health overall.

Additionally, many other treatment options are available to patients, including inhalers, medications, and surgical options.
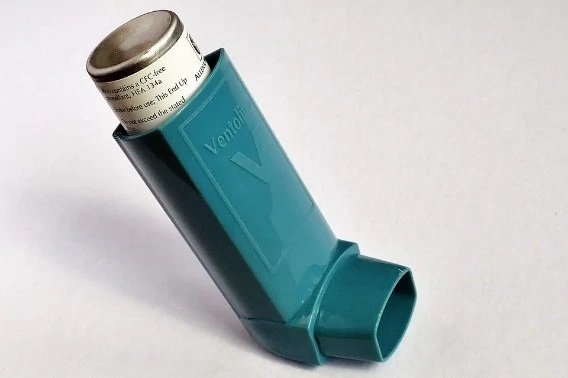
INHALERS FOR COPD
Unless you have asthma or another respiratory condition, you may think all inhalers are the same. However, there are quite a few different types with different specific purposes under the all-purpose goal of opening a patient’s airways.
COPD patients are sometimes prescribed more than one inhaler to address different symptoms.
The kinds of inhalers used to treat COPD include what are known as:
- Rescue inhalers
- Long-acting inhalers
- Anticholinergic inhalers
- Combination inhalers
Rescue inhalers are short-acting bronchodilators that offer fast relief when needed; these are not to be used daily but only in a case where extreme symptoms need to be alleviated quickly. They open up airways in just minutes, using medications such as albuterol.
Long-acting inhalers used to treat COPD would be used daily to control and relieve symptoms. They include salmeterol, formoterol, olodaterol, vilanterol, and the more recently FDA-approved indacaterol. These inhalers provide relief by relaxing the airways and helping patients with excess mucus in the lungs.
Long-acting inhalers do create unwanted side effects in some patients (such as headaches or jitters). Any side effects should be discussed with your doctor, who may be able to prescribe a different medication to treat COPD symptoms.
Another option in bronchodilators is an anticholinergic inhaler, which prevents muscle tightening around airways, making it difficult for COPD patients to breathe. The medicines anticholinergic inhalers (such as aclidinium, ipratropium, tiotropium, and umeclidinium) can be used in a nebulizer as well.
Finally, some combination inhalers offer COPD patients the benefits of bronchodilators along with inhaled corticosteroids, which are incredibly beneficial in reducing inflammation.
Combination inhalers can include:
- Bronchodilators + steroids
- Short-acting bronchodilators + anticholinergic
- Long-acting bronchodilators + anticholinergic
- Three long-acting medications: fluticasone, umeclidinium, and vilanterol
Getting the right combination to address your symptoms effectively may be a process of trial and error with your physician; be sure you follow all of the specific instructions associated with your inhaler and do not discontinue the use of a prescription without discussing it with your doctor first.
OTHER MEDICATIONS FOR COPD
In addition to inhaled medications as treatment for COPD, your doctor may prescribe other oral medications as well.
One medication that addresses lung tissue damage is roflumilast, which has been shown to improve lung function in COPD patients. However, it is typically reserved for individuals with a history of severe COPD. In addition, like many prescription medications, it can also come with unwanted side effects, such as headache, nausea, and dizziness.
Your healthcare provider will work with you to determine if an oral medication is right for you and monitor any other medications or supplements you take and how those could interact with your COPD treatment.
Individuals with COPD should always consult a physician before discontinuing the use of a medication or starting a new one.
SURGICAL OPTIONS FOR COPD
Lung transplantation is, in some cases, the final, lifesaving treatment option for COPD patients when breathing difficulties are severe. However, surgical treatments can be extremely complicated and will only be advised when your physician thinks it is your best option.
While lung transplants are a somewhat extreme option, there are also some less invasive options for COPD patients.
A bullectomy can be performed to remove damaged air sacs (or bullae) in the lungs; long volume reduction surgery may be performed to remove damaged or diseased lung tissue.
Another surgical option is endobronchial valve surgery, which is performed on patients with severe emphysema. In this procedure, valves are placed in airways to block off the sections of the lungs that are damaged. Then, the remaining parts of the lungs that are healthier will be able to work with greater efficiency, reducing breathing difficulties.
THE FUTURE OF COPD TREATMENTS
Advances in treatments for COPD are continually taking place thanks to clinical trials and modern research. As a result, future COPD patients may be treated with biologic drugs, which target inflammation.
Additionally, some clinical trials are investigating stem cell therapy in the treatment of COPD.
All of the newest treatment for COPD options, whether those currently available or ones that may be approved in the future, should be monitored by your physician, and tailored for your specific symptoms and progression.
Average Lung AirPhysio
ENJOY BETTER BREATHING - Use this 100% Drug Free Device - AIRPHYSIO
Recent Posts
Sports AirPhysio
IMPROVE YOUR SPORTING PERFORMANCE - Use this 100% Drug Free Device - AIRPHYSIO

AirPhysio Child
BETTER BREATHING FOR YOUR CHILD - Use this 100% Drug Free Device - AIRPHYSIO

Categories
- asthma (2)
- atelectasis (2)
- bronchiectasis (2)
- copd (3)
- cystic-fibrosis (45)
- featured (10)
- uncategorized (2)


